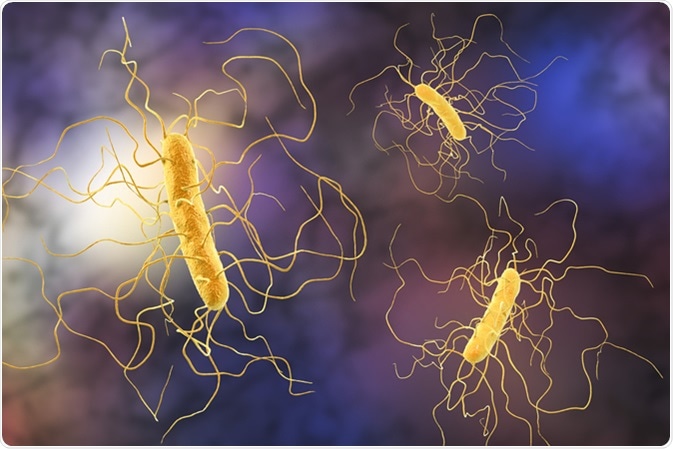
Clostridioides difficile infection (CDI or C-diff), also known as Clostridium difficile infection, is a symptomatic infection due to the spore-forming Clostridium difficile. Clostridioides difficile (formerly Clostridium difficile) colitis results from a disturbance of the normal bacterial flora of the colon, colonization by C difficile, and the release of toxins that cause mucosal inflammation and damage.
Antibiotic therapy is the key factor that alters the colonic flora. C difficile infection (CDI) occurs primarily in hospitalized patients. They decrease short-chain fatty acid absorption which results in osmotic, or watery, diarrhea.Complications may include pseudomembranous colitis, toxic megacolon, perforation of the colon, and sepsis.
Clostridioides difficile infection is spread by bacterial spores found within feces. Surfaces may become contaminated with the spores with further spread occurring via the hands of healthcare workers. Risk factors for infection include antibiotic or proton pump inhibitor use, hospitalization, other health problems, and older age. Diagnosis is by stool culture or testing for the bacteria’s DNA or toxins.
These infections mostly occur in:
- People 65 and older who take antibiotics and receive medical car
- People staying in hospitals and nursing homes for a long period of time
- People with weakened immune systems or previous infection with C. diff
- Symptoms might start within a few days or several weeks after you begin taking antibiotics.
Symptoms include:
- diarrhea: loose, watery stools (poop) for several days
- fever
- stomach tenderness
- loss of appetite
- nausea
- C. diff can easily spread from person to person.
Inactivation of Clostridium difficile
The source of health-care–associated acquisition of Clostridium difficile in nonepidemic settings has not been determined. The environment and carriage on the hands of health-care personnel have been considered possible sources of infection. Carpeted rooms occupied by a patient with C. difficile were more heavily contaminated with C. difficile than were noncarpeted rooms. Because C. difficile spore-production can increase when exposed to nonchlorine-based cleaning agents and the spores are more resistant than vegetative cells to commonly used surface disinfectants, some investigators have recommended use of dilute solutions of hypochlorite (1,600 ppm available chlorine) for routine environmental disinfection of rooms of patients with C. difficile-associated diarrhea or colitis, to reduce the incidence of C. difficile diarrhea, or in units with high C. difficile rates.
Stool samples of patients with symptomatic C. difficile colitis contain spores of the organism, as demonstrated by ethanol treatment of the stool to reduce the overgrowth of fecal flora when isolating C. difficile in the laboratory. C. difficile-associated diarrhea rates were shown to have decreased markedly in a bone-marrow transplant unit (from 8.6 to 3.3 cases per 1,000 patient-days) during a period of bleach disinfection (1:10 dilution) of environmental surfaces compared with cleaning with a quaternary ammonium compound. Because no EPA-registered products exist that are specific for inactivating C. difficile spores, use of diluted hypochlorite should be considered in units with high C. difficile rates.
Acidified bleach and regular bleach (5000 ppm chlorine) can inactivate 106 C. difficile spores in <10 minutes. However, studies have shown that asymptomatic patients constitute an important reservoir within the health-care facility and that person-to-person transmission is the principal means of transmission between patients. Thus, combined use of hand washing, barrier precautions, and meticulous environmental cleaning with an EPA-registered disinfectant (e.g., germicidal detergent) should effectively prevent spread of the organism.
Contaminated medical devices, such as colonoscopes and thermometers,can be vehicles for transmission of C. difficile spores. For this reason, investigators have studied commonly used disinfectants and exposure times to assess whether current practices can place patients at risk. Data demonstrate that 2% glutaraldehyde and peracetic acid, reliably kill C. difficile spores using exposure times of 5–20 minutes. ortho-Phthalaldehyde and > 0.2% peracetic acid (WA Rutala, personal communication, April 2006) also can inactivate >104 C. difficile spores in 10–12 minutes at 20ºC. Sodium dichloroisocyanurate at a concentration of 1000 ppm available chlorine achieved lower log10 reduction factors against C. difficile spores at 10 min, ranging from 0.7 to 1.5, than 0.26% peracetic acid with log10 reduction factors ranging from 2.7 to 6.0.
Tuesday, October 26, 2021
Refrences
Please Check out file at the following link
Quaternary Ammonium Compound Disinfectants